
Background:
Fasting during Ramadan is a fundamental pillar of Islam in which Muslims refrain from food and liquids as well as other activities. This is daily from sunrise to sunset and is one month long. Muslims fasting will typically have a large meal after their fast at sunset, and a further meal before sunrise. It is based on the lunar calendar and thus the start date changes by approximately 11 days each year when using the solar calendar (365 days). Thus, daylight hours can vary significantly between the Winter and Summer. Fasting days missed should be made up for outside of the month of Ramadan.
Engaging about medications and procedures with fasting Muslims can be challenging. For many, this will include for example, patients with diabetes mellitus or chronic kidney disease. Local anaesthetic (LA) procedures are common, and can broadly be divided into dental and non-dental. They include percutaneous or topical anaesthetic agents. Examples of where they are used includes skin lesion excisions, traumatic lacerations, peripheral injuries such as hands, vascular access procedures (e.g. angioplasty), and intra-oral or dental procedures. Given that patients will not be eating or drinking during this month, intra-oral or dental procedures require their own evaluation. Clinicians should be aware that many patients feel strongly about keeping their fasts where possible, including those considered exempt from fasting due to illness.
In this review, we give an overview of LA agents, explore religious rulings around fasting whilst undergoing LA procedures, and review any available safety data. Further to this, we discuss anticipated difficulties in speaking to Muslim patients about this. Importantly, we will give recommendations which health care providers can implement to maximise safety if patients do choose to fast. Discussion around tablet treatments, fasting with diabetes, and general anaesthetic (GA) procedures are not discussed here.
Local anaesthetic
A local anaesthetic (LA) is a reversible agent that typically works by blocking sodium channels and reducing or stopping afferent neuronal signals from sensory fibres (1). The decision to undertake a procedure under LA versus GA usually depends on the volume of LA required (e.g., a large versus small skin lesion), the presence of infection, and duration and type of procedure. Other factors such as surgeon and patient preferences play a role.
Infrequent side effects in high doses include neurological and cardiovascular depression, and thus maximum recommended doses exist. Lidocaine is the mostly widely used LA with a rapid onset within two minutes, and a duration of up to ninety minutes. Other commonly used LA agents such as Bupivacaine or Levobupivacaine have a longer onset of action (up to thirty minutes), however can last longer (up to 4-8hours) (2).
A prolonged duration of action can be beneficial due to the reduction in need for oral analgesics later on, which a fasting patient may decline. Addition of adrenaline provides a good haemostatic effect and allows use of higher doses of LA.
Religious rulings around local anaesthetic
The first and most important evidence in Islam comes from the Holy Quran. The verse below states that those who are ill are exempt from fasting.
“However, should any one of you be sick or on a journey, then (he should fast) a number of other days (equal to the missed ones)”
Surah Al-baqarah, Ayah 184, The Holy Quran. (Chapter Al-baqarah (The Cow), Verse 184)
A ruling on injections for medical purpose was passed by the Permanent Committee for Scholarly Research and Ifta/Fataawa al-Lajnah al-Daa’imah (10/252) (3). The Committee was established 1971 and is the main Islamic organisation in Saudi Arabia that passes issues rulings in Islamic jurisprudence.
“Being given medicine via injection does not break the fast, whether it is intramuscular or intravenous, so long as the injected substance does not provide nutrition, because in that case it is like food and drink which are forbidden to the one who is fasting”.
Through this, we can clarify to patients that injected LA agents, irrigation of wounds, sutures, and any antibiotic ointments, creams or dressings used after the procedure, are not a form of nourishment, and are necessary steps to ensure treatment of the condition.
Safety Data
The PubMed database was searched for articles relating to the safety of fasting specifically during Ramadan, and surgery. Although no formal data on the safety of LA procedures during fasting was found, this is generally thought to be safe. It is also discussed in a number of dental surgery publications. Related studies found are explored below, however with the caveat that many are based on studies outside the United Kingdom (UK).
Certain factors should be considered when planning a certain procedure whilst a patient is fasting. It would be unsafe to defer certain procedures such as skin cancer procedures, or traumatic lacerations. This is because risks such as infection, invasion, or metastasis may rise considerably. Clinicians should exercise a common-sense approach to this, for example, an elderly patient insistent on fasting with a relatively long local anaesthetic procedure may find this extremely challenging, and should be dissuaded from fasting if the procedure is urgent. Patients may also refrain from tablets and drinking small amounts of water with this, and thus analgesia and antibiotics can be challenging.
For ‘high-stake’ local anaesthetic procedures, e.g., percutaneous coronary intervention (PCI), our strong recommendation is to avoid fasting. This is because the potential for small complications to have significant effects is greater. One study investigating the safety of fasting during the first 3 month following PCI found this to be unsafe (4). Drawing on data from other larger procedures, a review of patients undergoing bariatric surgery around the month of Ramadan showed no increasing risk versus times distant from Ramadan (5). In a further prospective analysis in obesity surgery, more than 80% of patients changed the timing of their medications. Nearly 90% adhered to their prescribed medications (6).
At present, it remains unclear if fasting during Ramadan may benefit wound healing (7). There may be additional advantages for wound healing during Ramadan from patients smoking less during this period. There may also be immune advantages to fasting which could have implications for wound healing (8). Early post-operative nutrition may have a role in improving wound healing, and has led to Enhanced Recovery After Surgery (ERAS) protocols, including protocolised peri-operative nutrition for more major procedures (9). Care must be taken in years where Ramadan falls in the Summer months, where patients may be fasting greater than sixteen hours for part of the month. During this time, there may a risk of under-nutrition, rather than simple circadian-related fasting.
We advocate the use of a simple blood glucose measurement as a monitoring tool in patients undergoing LA procedures (e.g., lasting longer than fifteen minutes) whilst fasting, once at the beginning, and at any further clinical need, e.g., a suspected vasovagal reaction. Considerable efforts have been made to improve safety whilst fasting in diabetes mellitus, and this will usually be through the diabetic team.
For post-operative analgesia, we would recommend avoidance of non-steroidal anti-inflammatory drugs. This is due to the association of fasting with perforated peptic ulcers (10, 11). Oral paracetamol and weak/moderate opioids (e.g. codeine) are usually sufficient if required post-operatively.
Management of patients with chronic conditions such as diabetes mellitus or adrenal disease during Ramadan is complex. A very useful summary traffic light table for when it may be acceptable or unacceptable for patients with chronic conditions to fast can be found through the British Islamic Medical Association (BIMA) Rapid Ramadan Review (12). Where possible, advice should be undertaken through discussion with respective sub-specialities. For patients taking anticoagulation, evidence for INR change is mixed between within the therapeutic range, below this, or raised (13-16). In the study of 32 patients where INR was found overall to be raised, no bleeding or thrombotic events were reported (14). Thus, INR should be checked prior to local anaesthetic surgical procedures. Fasting may reduce the efficacy of clopidogrel in diabetic patients (17).
Medical Emergencies during LA procedures
Medical emergencies that may occur during LA procedures include anaphylaxis, asthma, cardiac emergencies, epileptic seizures, hypoglycaemia, adrenal insufficiency, and syncope. Almost without exception, these conditions will necessitate administration of medication immediately (e.g. adrenaline injection in the case of anaphylaxis), or immediately after the initial event has taken place (e.g. diazepam injection in the case of prolonged epileptic seizures). Islamic rules governing fasting are very clear; one of the acceptable reasons for breaking the fast is if life is threatened. Thus, if a person has a condition that is a threat to his or her life (e.g. poorly controlled diabetes), it is forbidden by Islamic law for them to continue fasting (18-21).
The most common medical emergency during dental treatments in healthy fasting patients is a hypoglycaemic attack. The onset of the attack can be triggered by the increased stress level during dental treatment or during administering the LA agent. The signs and symptoms of a hypoglycaemic attack include shaking/trembling, slurred speech or vagueness, sweating and pallor, blurred vision, tiredness/lethargy, confusion/aggression, and in severe cases, loss of consciousness. The management of a hypoglycaemic attack should be done using an ‘ABCDE’ approach, and usually involves the use of buccal/oral glucose gels, intramuscular glucagon, or IV glucose, as per local policy. The patient should not continue their fast after this.
As a recommendation, it is advisable to defer any dental treatments in diabetic patients until either after they break their fast (iftar), or after Ramadan where possible (22).
Surgical Skin and Hand Procedures (non-dental procedures) :
In this section we explore non-dental procedures. The range of percutaneous procedures is large. This includes for example, excision of skin lesions, repair of traumatic lacerations, hand and upper limb procedures, pacemaker insertion, and vascular procedures, e.g. angioplasty. The recommendation is not to fast during ‘high stake’ procedures, such as during or after percutaneous coronary intervention (4). Throughout all of these, shared decisions should be made with the patient. Some specific pieces of guidance are included below.
Traumatic Lacerations
In trauma scenarios, patients may present to the emergency department, or trauma clinics with lacerations, for example a forehead laceration after a fall. After excluding more significant injury, e.g. head trauma in a forehead laceration, such lacerations can be managed in a standard fashion, and patients should be counselled that the local anaesthetic, irrigation, and sutures do not constitute nourishment. It would be impractical to delay closing such laceration to after Ramadan, unless in the final day or two. Typically, traumatic hand lacerations should be operated on within four days, e.g. flexor tendon repair (23). Furthermore, the risk of infection, desiccation of the underlying tissues, and an unsightly scar may rise. Procedures can be postponed to after sunset, though we would not advocate this, as it encroaches on the emergency night on call teams’ time, and expertise may be less readily available should there be complications. We would advocate the use of absorbable sutures to reduce hospital/ GP visits during the fasting month. Research shows no difference in cosmetic results in facial lacerations (24). If antibiotics are required, we would advocate the use of those requiring less frequent administration, e.g. clarithromycin as a twice daily dose. For clean small lacerations, e.g. facial, topical agents such as chloramphenicol ointment may replace the need for oral antibiotics as well as dressings. Discussions around topical medications are also important, as their use may also be rejected by some patients (25). In hand surgery, for simple wounds that have been thoroughly cleaned during a minor procedure, evidence is emerging for avoiding routine use of prophylactic antibiotics (26).
In hand and upper limb surgery, procedures may be undertaken under regional (e.g axillary block, digital ring block) or local field block. A consideration with regional anaesthetic is that patients usually are required to fast, as if this is unsuccessful (typically <5% of patients), then this may need to be converted to a general anaesthetic. Wide Local Anaesthetic with No Tourniquet (WLANT) (27) is a technique that is becoming more popular within many hospitals across the UK. This technique eliminates the need for GA or regional anaesthetic, and often patients are discharged the same day.
Elective Procedures
In elective scenarios, more time may be available to have more detailed discussions with patients, and allow them to consult family or local religious leaders. Skin lesions requiring minor procedures may be benign or malignant. Common benign condition includes cysts, lipomas, and benign naevi. Criteria warranting urgent operations includes incision and drainage of small abscesses (e.g. infected sebaceous cyst), symptomatic lesions (where malignancy is a differential), or those causing nerve compression. Otherwise, the vast majority of simple skin procedures can be delayed until after Ramadan, should patients find LA minor procedures on these unacceptable during the fasting period.
Skin cancers are the most common cancer in UK with 152,000 cases of non-melanoma skin cancer cases per year and over 16,000 melanoma cases (28). The most common subtype is a basal cell carcinoma (BCC); a slow growing; locally invasive skin tumour (28). Although there are a number of modalities of treatment, standard surgical excision under LA as day case procedure, is the most common. BCC usually does not metastasise, and longer waiting times may be more acceptable versus other more aggressive skin malignancies, such as squamous cell carcinoma (SCC), melanoma, or merkel cell carcinoma (29). Thus, patients may opt to wait until after Ramadan. The remaining diagnosis may require reconstruction with either a full thickness skin graft or a local flap. Ensure long acting LA is used for skin graft donor areas, e.g. over the kaltostat dressing. This is to reduce post-operative discomfort/pain and need for oral analgesia (30).
Elective cases include carpal tunnel decompression, trigger finger release, joint replacement, Dupuytren’s disease excision, tenolysis, scar contracture release/full thickness skin graft, and ganglion excision (31-34). All of these cases can be considered under local, WALANT, or regional block. Patients may also be given extra dressings to take home with advice on how to use them. This may avoid the need for further checks at the GP or dressing clinics during fasting period.
Other procedures
Other procedures e.g. angioplasty or pacemaker insertion are routinely undertaken under local anaesthetic. This typically involves the radial or femoral arteries for access. Given the significance of the undertaken, i.e. a functional cardiac procedure, we would not advocate that patients fast during such more ‘major’ procedures. LA for Ophthalmic operations, e.g. laser eye surgery (vision correction), may be rejected by some patients (35).
Recommendations for non-dental procedures:
• Patients should be talked through the expected operative and post-operative period, and a shared decision should be made, with respect for the patient’s autonomy.
• Utilise long acting LA agents to reduce the need for post-operative analgesia. If antibiotics are required, consider those with less frequent administration schedules.
• Any suspicious lesions i.e. SCC, Melanoma should still be treated urgently, and the urgency should be stressed to patients who do not find local anaesthetic procedures acceptable during Ramadan.
• LA procedures that should not fast include regional anaesthetic e.g. axillary block for upper limb procedures, and minor procedures on infected wounds, especially those requiring oral antibiotics at a particular dosing regimens.
Dental Procedures
Summary of recommendations for dental procedures:
● Most patients would consider substances entering through the oral route to break their fast.
● Encourage fasting patients to visit their dentists well before Ramadan to anticipate early any dental work needed.
● Some dental treatments such as simple restorations, scaling and polishing, cosmetic treatments, and any non-emergency treatments, can be deferred until after Ramadan with a shared agreement between the patient and dentist.
● Deferring any dental treatment until after the breaking of the fast after the sunset is recommended where possible, as it will increase patient’s comfort and reduce the worry of swallowing any substances.
● Alongside the new recommendations for infection control and reducing the transmission of COVID-19, it is always recommended to use a dental rubber dam during any dental procedure wherever possible. This will also reduce the chances of the patient accidentally swallowing any substances.
• If a patient requires antibiotics, consider a less frequent regime.
• Chlorhexidine mouth wash that is commonly prescribed may not be adhered to as fear it of swallowing it; discuss with patient their concerns and if reluctant, advise use outside of fasting. This would also be the case for toothpaste.
Substances entering the mouth is likely to make fasting patients believe this will void their fast, as it is the route by which food and fluid enters the body. Due to this fear, patients may only present in emergency scenarios due to inability to tolerate the pain. Patients may fear that inadvertent swallowing of spray from procedures such as scaling, intraoral administration of anaesthetics, or accidental swallowing of the saliva during a routine examination or restoration placement will break their fast. Hence, they may refrain from seeking dental treatment (18). Teeth with small cavities can be temporised with temporary dressings, as long as it proves asymptomatic, and the definitive treatment like placement of the final restorations can be delayed safely till after Ramadan. The patient must be made fully aware if a definitive treatment is needed as soon as practical.
Oral hygiene maintenance
Chlorhexidine is a commonly prescribed antiseptic mouthwash usually used for very specific indications and for a short period of time. It may be used as a mouthwash, spray, or gel for a variety of conditions. Patients may be reluctant to use any mouthwash for fear of absorption from the mucosa and of inadvertently swallowing some. Patients should be advised that again this does not provide a form of nourishment, and has the intention of aiding in treatment or preventing a disease. It may be advisable to discuss these issues with the patient concerned and to suggest that, if the patient is reluctant to use the mouthwash during the fasting period, he or she should use it outside fasting hours, especially taking into account that Chlorhexidine mouthwash dose is usually 10mls twice daily, and can be used before starting the fast (fajr) and after breaking the fast (iftar) and (36). Fasting patients will rinse their mouths out with water throughout the day as part of their cleaning regime for prayers.
It is good practice to brush the teeth twice daily with high Fluoridated toothpaste, once before starting the fast (before the sunrise), and the second time whenever possible. To reduce worries about swallowing tooth paste, the second time can be performed after breaking the fast (iftar) meal.If brushing is carried out during fasting, then you can advise patients to rinse with water to remove any toothpaste that may cast doubt on their fast. Patients who brush outside of fasting hours should be advised to spit the toothpaste and not rinse with water after brushing as per usual.
Benzyl isothiocyanate is the active antimicrobial agent in Salvadora persica (siwak) widely used in Islamic countries for oral hygiene. Usage of Siwak was advised and recommended by the Prophet Mohammed during fasting. The original Siwak chewing stick has antimicrobial effects similar to toothbrushing with general toothpaste and Salvadora persica toothpaste by reducing the numbers of Strepococcimutans and Lactobacilli Colonies, which is considered the main bacteria responsible for tooth decay (37).
Treatment considerations
Treatment procedures such as scaling, restorations, and extractions with LA do not invalidate the Ramadan fast, with a minimal risk of swallowing substances (38). Other treatment procedures, such as application of varnishes for caries control, are better avoided in apprehensive patients, where alternative treatment options should be selected. Pulp capping which involves placing a medicament directly over the pulp, can still be carried out as it does not interfere with fasting.
Local Anaesthetic Injections
This is an acceptable form of treatment for a fasting patient (18, 36); however, the dentist should be aware that some Muslim patients may be reluctant to undergo it. According to Islamic fatwa, administration of LA for dental treatment does not invalidate the fast (39). If a long-acting LA is used, the need for analgesics may be reduced, as discussed above. Moreover, evening (after iftar) appointments will permit patients to avoid the need for analgesic intake until they can break their fast, however this is specific to individual practice opening times.
Intravenous Injections
Intravenous (IV) injections are generally permissible whilst fasting (3, 18, 36). IV Midazolam, for example, is commonly used for sedation in anxious patients, mainly in secondary and tertiary care settings. However, the use of IV fluids for nutrition is prohibited while fasting as it provides a significant source of nourishment to the fasting patient (36).
Minor Oral Surgeries
Where possible, fasting patients undergoing a dental extraction during the month of Ramadan should discuss with their dentist other treatment options like temporary dressings. Dental extractions, however, can be carried out for immediate pain relief without violating a patient’s fast if preventive measures such as high-vacuum suction tips are used. Fasting patients should be aware that analgesics are likely to be needed once the LA effect has worn off.
A supine position is indicated as it prevents syncope. Swallowing of blood as well as the possible need for antibiotics or strong analgesics following the removal of a tooth in case of surgical extraction, will invalidate the fast. Hence, pulpal extirpation can be carried out as an alternative to tooth extraction. If pulpal extirpation is performed, high-volume suction, rubber dam, and an upright position should be used to prevent swallowing (40). Extractions can be followed by placement of sutures. Sutures will minimise the risk of blood/saliva swallowing and hence lower the risks of invalidating the fast.
Some facial dentally-related swellings must be managed urgently as these can be life-threatening, e.g. dental abscesses affecting the airway. Localised dental abscesses can be enclosed by the gums around the root of the infected tooth. The management of such cases is to provide an immediate drainage pass to the pus by an intraorally performed incision under LA. Delivering this treatment can provide an immediate relief of the patient’s symptoms, however, during the drainage, the patient should be assured that the pus will be collected and removed by high-volume suction and kidney trays to prevent any swallowing. However, some swellings can diffuse into the facial spaces and can be large, necessitating the need sometimes for a GA incision and drainage and IV antibiotics. Thus, breaking the fast in these cases is recommended as it’s considered life-threatening. (18-21).
Topical Fluoride Applications
Fluoride application is often used for prevention of dental caries and also as a treatment for tooth sensitivity. In either case, the fasting patient may be reluctant to accept this treatment, the concern being that he or she could inadvertently swallow the varnish or paste. Dentists should thus recommend that adjunctive treatment is carried out outside the hours of fasting. (36).
It is worth noting that some fluoride varnishes contain alcohol. It has been agreed, however, on the authority of the West Midlands Shari’ah Council, that these are suitable for use by Muslims, as long as it is used as a medication, and not as an inebriant. Furthermore, they should be used in minimal amounts, less than that which would inebriate, and they are not being used for reasons of conceit (41).
Alternatively, Super Fluoride toothpaste can be prescribed to patients at high risk of dental caries. Where the patient is aged 10 and above, a sodium fluoride 2800 PPM is recommended. In addition, a higher dose (sodium fluoride 5000 PPM) is indicated if the patient suffers from root caries, dry mouth, or a highly cariogenic diet or medication. This later higher dose can only be prescribed to patients aged 16 and above (41).
Both toothpastes can be very useful to compensate the use of Fluoride varnish if the patient does not want to opt for these during Ramadan. It is expected that the patient should brush twice per day, once in the morning, and the last thing before going to bed, and for the fasting patient, once immediately before starting the fast (after suhoor), and the second after the main meal when breaking their fast (41).
Topical Gels and Lozenges
Intra oral gels and lozenges are mainly prescribed for ulcers, oral thrush, and denture stomatitis. If this is applied during the fasting hours, it will invalidate the fast, due to swallowing the medication. Therefore, compliance with these medications is likely to be poor in patients adamant about fasting. Thus, it is recommended to schedule these medications after fasting hours (36).
Oral Medications
Patients may fear that medications taken orally will break their fast. However, if the person becomes ill during the fasting period, it is permissible to break the fast. It is the patient who has to judge the degree of illness. If the illness is life threatening, the patient is advised to take the required medication.
One study observed that 42% of Muslim patients followed their regular drug regimen during Ramadan, however, 58% changed their intake pattern (42). Patients may resort to taking a large, single dose during the feasting hours or may even miss a dose. This behaviour increases the risk of drug toxicity, and this effect is more pronounced in the elderly. Dental treatment or emergency management of a condition may require the dentist to prescribe oral medications. However, since the fasting patient cannot take medications during periods of fasting, the drug regimen can be altered.
Use of a single daily dose can be advantageous in patients who have an evening dosing schedule. In cases where single dosing is not possible, the number of doses can be reduced by using slow-release or chronotherapeutic formulations, or drugs with a longer elimination half-life. An example of such a substitution is the use of amoxicillin instead of penicillin. Amoxicillin requires 3 daily doses in contrast to penicillin, which requires administration 4 times per day. (40, 42).
Transdermal Post-Operative Analgesia
Transdermal drug delivery, for example, a transdermal patch of diclofenac or tramadol, serves as a replacement for the traditional dosing system, avoiding the need for an oral route of drug administration. The drug contained within a delivery patch diffuses through the intact skin, reaching the vasculature underneath for systemic delivery of the drug. This method offers several advantages. It is not taken orally and hence should not interfere with fasting, however again respect for patient autonomy should be exercised (25). Moreover, other potential side effects of drugs, such as gastric irritation, are eliminated. Transdermal delivery also provides a steady state of drug delivery. This method of drug dosing can be applied to overcome post-extraction or post-flap oral pain. (43, 44).
The efficacy of transdermal patches following extractions has been well documented. In one study, transdermal patches containing 100 mg of diclofenac used once daily were compared to 50 mg of oral diclofenac administered 3 times per day. The usage of a transdermal patch brought about significantly greater pain reduction than did oral diclofenac (45).
Summary of Dental Procedures
Some Muslims patients may wrongly perceive that all dental treatments and preventive procedures invalidate the fast, even though most dental treatments will not break the fast. This includes scaling, restorations, and extractions. However, some patients may not be willing to carry out certain procedures due to different perceptions and opinions. Within the month of Ramadan, most forms of prescribing are allowable, with the notable exception of oral medication. Even with acceptable types of medication, the patient will often find open or hidden reluctance to comply with the regimen prescribed. The healthcare professional must be aware of this and should alter their prescribing practice or advice accordingly.
It is also important, when treating a fasting patient on long term medication, to ensure satisfactory compliance with the normal drug therapy. With fasting patients in dental practice, it is important for professionals to be aware of which treatments the individual considers acceptable and offer treatment accordingly.An understanding of the effects of prolonged fasting and knowledge of dosing recommendations will help dentists in treatment planning of medically compromised patients during Ramadan. In addition, various alternative dental treatment approaches that are regarded as permissible during fasting have also been described.
We have summarised these recommendations in a flow chart for guidance for dental care professionals to help them identify patients’ needs and their management based on a risk assessment approach (Figure 1).
Summary of recommendations:
Besides the highlights of the recommendations in figure No1, we would summarise our recommendations as follows:
● Respect must be maintained for a patient’s individual views and decisions. Patients should be offered the opportunity to speak to relatives, local imams, and do their own research. A shared decision should be made.
● Patients with a form of illness are expected to be exempt from fasting. If patients are adamant about maintaining their fast, extra-oral local anaesthetic (LA) does not usually interfere with fasting as it is not nourishing and intended as part of treatment.
● Where possible, procedures should be deferred to after Ramadan if patients feel strongly about keeping their fast. Risks of delaying procedure should be discussed with the patient.
● A blood glucose reading should be checked in fasting patients undergoing LA procedures. Patients taking warfarin should have their INR checked prior to any minor surgical procedures.
● Hospital procedures should not be undertaken out of daylight hours based on patient preference, due to the reduced availability of staff in hospitals to assist with complications in daytime versus night-time.
● Mixed short and long-acting LA agents should be used to provide rapid onset and an extended duration of action, minimising the potential need for oral analgesics later on.
● Use antibiotics (prophylactic or therapeutic) with less frequent dose regimes, to improve the chances of patient compliance, e.g., twice daily versus three or four times daily.
Conclusions
In summary, patients must be counselled appropriately, and involved in the decision-making process at all stages of the treatment. This should be informed. Various steps, as described above, may be taken to improve the safety and success of treatments in patients who choose to continue fasting whilst undergoing local anaesthetic procedures.
Many thanks to the following who contributed in reviewing the recommendations:
– Mr. Mogdad Alrawi, Consultant Plastic Surgeon, Newcastle
– Mr. Zaki Shariff, Consultant Plastic Surgeon, Bradford
– Dr. Anas Nasahawi, Dentist & Oral Surgeon, Lincolnshire
– Dr Ihab Ibrahim, Dentist, Leeds
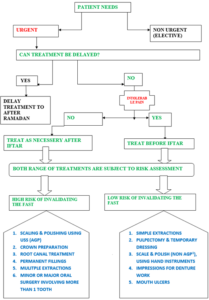
(Figure No. 1, shows management of patient needs during Ramadan using risk assessment based approach)
1AGP: Aerosol Generating Procedure
*Please note that this is only a guidance and exhaustive risk assessment is to be carried out by the clinician.
References
1. Becker DE, Reed KL. Local anesthetics: review of pharmacological considerations. Anesth Prog. 2012;59(2):90-10
2. https://emedicine.medscape.com/article/873879-overviewa5. Accessed: 20.2.2021
3. https://islamqa.info/en/answers/65632/does-having-an-anaesthetic-via-injection-during-ramadaan-break-the-fast. Accessed 16/2/2021
4. Amin OA, Alaarag A. The safety of Ramadan Fasting following Percutaneous Coronary Intervention. BMC Cardiovasc Disord. 2020 Nov 19;20(1):489. doi: 10.1186/s12872-020-01784-8. PMID: 33213367; PMCID: PMC7678075.
5. Tat C, Barajas-Gamboa JS, Del Gobbo GD, Klingler M, Abdallah M, Raza J, Abril C, Corcelles R, Kroh M. The Effect of Fasting during Ramadan on Outcomes after Bariatric Surgery at an Academic Medical Center in the Middle East. Obes Surg. 2020 Nov;30(11):4446-4451. doi: 10.1007/s11695-020-04844-2. Epub 2020 Jul 13. PMID: 32661957.
6. Al-Ozairi E, Al Kandari J, AlHaqqan D, AlHarbi O, Masters Y, Syed AA. Obesity surgery and Ramadan: a prospective analysis of nutritional intake, hunger and satiety and adaptive behaviours during fasting. Obes Surg. 2015 Mar;25(3):523-9. doi: 10.1007/s11695-014-1373-0. PMID: 25595382.
7. Hayati F, Maleki M, Pourmohammad M, Sardari K, Mohri M, Afkhami A. Influence of Short-term, Repeated Fasting on the Skin Wound Healing of Female Mice. Wounds. 2011 Feb;23(2):38-43. PMID: 25881054.
8. Latifynia A, Vojgani M, Gharagozlou MJ, Sharifian R. Neutrophil function (innate immunity) during Ramadan. J Ayub Med Coll Abbottabad. 2009 Oct-Dec;21(4):111-5. PMID: 21067041.
9. Abela G. The potential benefits and harms of early feeding post-surgery: a literature review. Int Wound J. 2017 Oct;14(5):870-873. doi: 10.1111/iwj.12750. Epub 2017 Mar 29. PMID: 28371381.
10. Torab FC, Amer M, Abu-Zidan FM, Branicki FJ. Perforated peptic ulcer: different ethnic, climatic and fasting risk factors for morbidity in Al-ain medical district, United Arab Emirates. Asian J Surg. 2009 Apr;32(2):95-101. doi: 10.1016/S1015-9584(09)60018-X. PMID: 19423456.
11. Golash V. Ten-Year Retrospective Comparative Analysis of Laparoscopic Repair versus Open Closure of Perforated. Oman Med J. 2008 Oct;23(4):241-6. PMID: 22334835; PMCID: PMC3273918.
12. https://britishima.org/ramadan-rapid-review/
13. Yildirim E, Secen O, Uku O, Nail Bilen M, Kutlu Karadag M. Is Fasting for Ramadan Safe in Patients with Mechanical Cardiac Valves? J Heart Valve Dis. 2017 Mar;26(2):200-204. PMID: 28820550.
14. Lai YF, Cheen MH, Lim SH, Yeo FH, Nah SC, Kong MC, Mya D, Lee LH, Ng HJ. The effects of fasting in Muslim patients taking warfarin. J ThrombHaemost. 2014;12(3):349-54. doi: 10.1111/jth.12496. PMID: 24354801.
15. Awiwi MO, Yagli ZA, Elbir F, Aglar AA, Guler E, Vural U. The effects of Ramadan fasting on patients with prosthetic heart valve taking warfarin for anticoagulation. J Saudi Heart Assoc. 2017 Jan;29(1):1-6. doi: 10.1016/j.jsha.2016.06.004. Epub 2016 Jun 15. PMID: 28127212; PMCID: PMC5247300.
16. Sridharan K, Al Banna R, Qader AM, Husain A. Does fasting during Ramadan influence the therapeutic effect of warfarin? J Clin Pharm Ther. 2021 Feb;46(1):86-92. doi: 10.1111/jcpt.13254. Epub 2020 Sep 14. PMID: 32926452.
17. Bouida W, Baccouche H, Sassi M, Dridi Z, Chakroun T, Hellara I, Boukef R, Hassine M, Added F, Razgallah R, Khochtali I, NouiraS; Ramadan Research Group. Effects of Ramadan fasting on platelet reactivity in diabetic patients treated with clopidogrel. Thromb J. 2017 Jun 2;15:15. doi: 10.1186/s12959-017-0138-0. PMID: 28588426; PMCID: PMC5457725.
18. 18 – Darwish S. The management of the Muslim dental patient. Br Dent J. 2005;199(8):503.
19. Sheikh A, Gatrad AR. Caring for Muslim Patients. Kannur (Cannanore), Kerala: Radcliffe Medical Press; 2000.
20. Khan FA, Williams SA. Cultural barriers to successful communication during orthodontic care. Community Dent Health 1999;16:256 61.
21. Trepanowski JF, Bloomer RJ. The impact of religious fasting on human health. Nutr J 2010;9:57.
22. Basic guide to medical emergencies in the dental practice / Phil Jevon ; consulting editors, Celia Strickland, Tessa Meese, Jagtar Singh Pooni.
23. Philip Jevon author. Celia Strickland, editor.; Tessa Meese, editor.; J. S Pooni, editor.
24. Chichester, West Sussex, UK : Wiley Blackwell: Second edition.: 2014
25. Gillanders Et al. A systematic review and meta-analysis: Do absorbable or non-absorbable suture materials differ in cosmetic outcomes in patients requiring primary closure of facial wounds? JPRAS 2018
26. Patel T, Magdum A, Ghura V. Does fasting during Ramadan affect the use of topical dermatological treatment by Muslim patients in the UK? Clin Exp Dermatol. 2012 Oct;37(7):718-21. doi: 10.1111/j.1365-2230.2012.04403.x.Epub 2012 Jun 8. PMID: 22681415.
27. G. R. F. Murphy et al. Meta‐analysis of antibiotics for simple hand injuries requiring surgery. BJS. 2016
28. Lalonde D. Wide Awake Local Anaesthesia No Tourniquet technique (WALANT). BMC Proc. 2015
29. https://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/non-melanoma-skin-cancer. Accessed 17.2.2021
30. Telfer Et al. Guidelines for management for Basal cell carcimona. British journal of dermatology 2009.
31. Desai C et al. Effectiveness of a topical local anaesthetic spray as analgesia for dressing changes: a double-blinded randomised pilot trial comparing an emulsion with an aqueous lidocaine formulation. Burns. 2014
32. Lichtman DM, Florio RL, Mack GR. Carpal tunnel release under local anesthesia: evaluation of the outpatient procedure. The Journal of Hand Surgery, 01 Nov 1979, 4(6):544-546
33. D.M.Eastwood, K.J.Gupta, D.P.Johnson, Percutaneous release of the trigger finger: An office procedure. The Journal of Hand Surgery. Volume 17, Issue 1, January 1992, Pages 114-117
34. Denkler, Keith. Dupuytren’s Fasciectomies in 60 Consecutive Digits Using Lidocaine with Epinephrine and No Tourniquet. Plastic and Reconstructive Surgery: March 2005 – Volume 115 – Issue 3 – p 802-810
35. Jin Bo Tang, Wide-Awake Primary Flexor Tendon Repair, Tenolysis, and Tendon Transfer. Clinics in Orthopedic Surgery 2015;7:275-281.
36. Kumar N, Jivan S. Ramadan and eyedrops: the muslim perspective. Ophthalmology. 2007 Dec;114(12):2356-60. doi: 10.1016/j.ophtha.2007.04.031. PMID: 18054644.
37. Khalid A, Raman B Transcultural oral health care: Dental medication for muslim patient. Dent Update 2000; 27:449 52.
38. ErlinaSihMahanani, MohdFadhli Khamis, ErryMochamadArief, Siti Nabilah Mat Rippin, Zainul Ahmad Rajion. Antibacterial efficacy of Salvadora persica as a cleansing tooth towards Streptococcus mutans and Lactobacilli colonies. Dental Journal (MajalahKedokteran Gigi)
39. PeedikayilFC, Thomas A, Naushad MC, Narayan A. Management of Muslim dental patient while fasting. Eur J Gen Dent. 2014;3(1):82-84.
40. Fatwa on Local anaesthetic by sheikh ibn Baz
accessed 28.1.2021
https://islamqa.info/en/answers/95062/anaesthetic-does-not-break-the-fast
41. Uppal N, Shikha D. Minor oral surgery in fasting Muslim patients during Ramadan [letter]. J Can Dent Assoc. 2013;79:d155.
42. Delivering better oral health: an evidence-based toolkit for prevention
43.https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/605266/Delivering_better_oral_health.pdf
44. Adil N, Houti IE, Moussamih S. Drug intake during Ramadan. BMJ. 2004;329(7469):778-782.
45. Bhaskar H, Kapoor P, Ragini. Comparison of transdermal diclofenac patch with oral diclofenac as an analgesic modality following multiple premolar extractions in orthodontic patients: a cross over efficacy trial. Contemp Clin Dent. 2010;1(3):158-163.
46. Tejaswi DV, Prabhuji ML, Khaleelahmed S. Comparative evaluation of transdermal diclofenac patch and oral diclofenac as an analgesic modality following root coverage procedures. Gen Dent. 2014;62(4): 68-71.
47. Prithvi S. Bachalli, H. Nandakumar , N. Srinath. A comparitive study of diclofenac transdermal patch against oral diclofenac for pain control following removal of mandibular impacted third molars. Journal of Maxillofacial and OralSurgery volume 8, pages167–172(2009)

